Are you missing most or all of your teeth? You may be able to restore a strong smile through the use of full-arch dental implants in Palo Alto and Redwood City. Depending on your bone loss level, your dentist may opt for an all-on-4 or all-on-6 dental implant.
Read on to learn more about these common dental implants in Redwood City, CA, and how they differ from traditional custom implants.
All-on-4 Same Day Implants
If you want to replace your whole lower and upper set of teeth, consider getting all-on-4 implants in Redwood City. It could be All-on-5 or 6 as well.
Your dentist will put four zirconium implants in your available bone. Then, they will add abutements that can hold temporary replacement teeth.
The good thing about this type of implant is that the procedure can be done over the course of a single dental appointment. Yes, you heard it right. You can get all-on-4 same-day implants in Palo Alto or Redwood City. The artificial roots and your temporary replacement teeth are fixed on the same day.
Pros
- Looks and Feels Real: All-on-4 implants look and feel like your natural teeth. Although getting accustomed to them may take some time, you won’t notice any difference eventually.
- Speed of treatment: They don’t call them “same day” implants for nothing. The surgery, bone grafting, and implant placement are all completed in a day. The surgery is minimally invasive and carried out with the aid of anesthesia.
- Quick Healing Process: The nature of the all-on-4 implants in Redwood City allows for speedier healing than traditional implants. Most patients can resume work within a few days without relying on strong medication. And the four zirconium implants start integrating with your jawbone from day one.
- Easy to Clean and Maintain: All-on-4 implants create no new dental chores for you. Just brush twice a day using non-abrasive toothpaste. It is also cruel to floss around the implants. Bi-annual dental checkups are recommended for evaluating overall oral health.
Cons
- Learning to Speak: All-on-4 dental implants eventually feel and look like your real teeth, but there’s a learning curve. Immediately after the procedure, you may find it a bit difficult to speak.
- Not Suitable for Everyone: Patients with extensive bone loss may not be eligible for all-on-4 implants in Redwood City
Custom Implants with Bridges and Crowns
Custom dental implants are considered the gold standard in dental implants and are ideal for patients missing one, or few teeth or entire arches. This procedure requires several appointments with a top dental implant dentist in Redwood City.
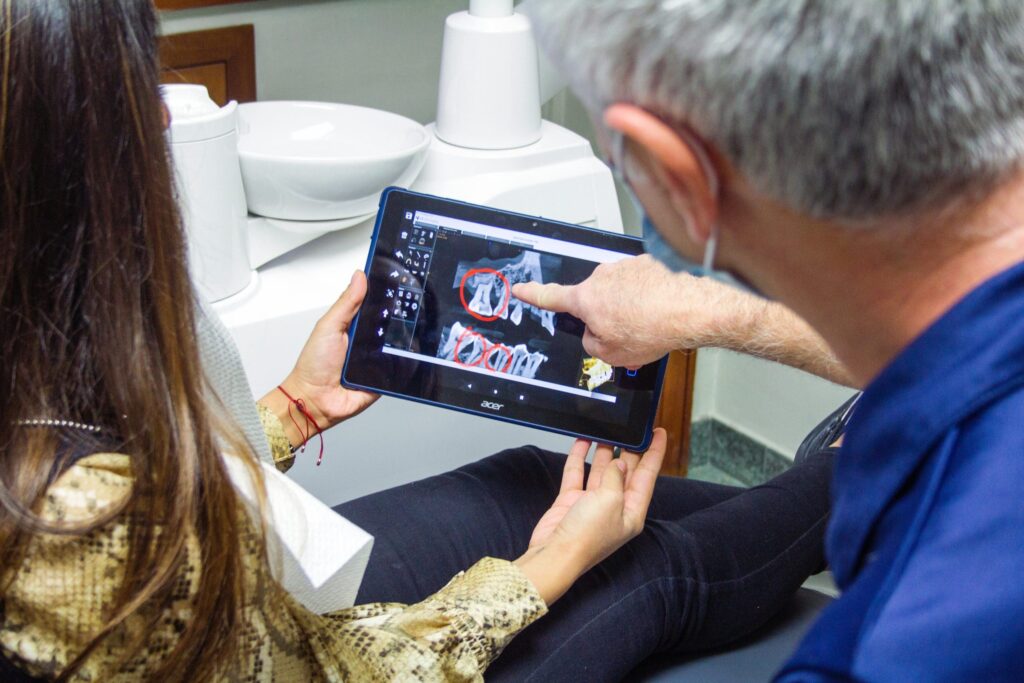
During your first appointment for this procedure, the dentist will take digital X-rays to be used as a basis for your customized treatment plan. Next, the dentist will insert a titanium rod into your jawbone.
After the rod has fully healed and the grafting process is complete, the dentist places an abutment that supports the crown (new tooth).
Pros
- Looks and Function like Natural Teeth: Custom dental implants resemble natural teeth, allowing you to speak, eat, and smile with confidence.
- Preservation of Bone and Facial Structure: Custom implants preserve the jawbone’s integrity. Also, they prevent bone loss commonly associated with missing teeth.
- Long Lasting: Custom dental implants can last a lifetime when well taken care of.
- Easier Oral Hygiene: Custom implants can be flossed and brushed like natural teeth.
Cons
- Lengthy Healing Process: Implants can take 3 – 6 months to integrate fully (osseointegration) with the bone tissue. Therefore, you must be watchful of your oral habits during this healing period. However, dentists will always advise you on the dos and don’ts after the procedure.
- Not everyone is a Suitable Candidate. Good candidates must have healthy gums and adequate bone density to support the implant. Visit the best dental implant dentist in Palo Alto to help you determine your eligibility.
Which Option is Better?
Which option should you choose? While all-on-4 implants and custom dental implants both replace missing teeth, there are various crucial differences.
For instance, getting all-on-4 same-day implants is faster. It can be completed in a single sitting. On the contrary, custom dental implants require several appointments.
Also, the all-on-4 procedure is a faster procedure but if you are looking for a solution that most closely matches your natural teeth in looks and functionality, a custom implant with bridges and crowns is a better solution for you.
That said, if you are not sure which the best option is, contact the dental implant dentists at Blue Turtle Dental. We will evaluate your current oral condition and recommend the best treatment plan.